We sure do have a confusing relationship with weight and food in our country. On one hand, we herald those who are thin and fit; but then look at the enormous availability of pre-packed, processed food that is ripe and ready for the picking 24 hours a day, seven days a week for anyone living in this country.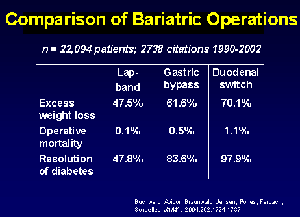
When it comes to those who are overweight or obese, our compassion flies out the window as quickly as we can toss that burger wrapper in a nearby garbage can. As obesity reaches epidemic proportions and weight-related conditions like diabetes and heart disease are starting to be diagnosed in younger and younger people, science has started to redefine and rethink its long-held hypotheses on obesity. Namely, that obesity, just like other inherited diseases, is hereditary. Even though, we still don’t have the grasp on the precise mechanism for how obesity becomes expressed, we do know that a variety of biological, environmental, social and psychological factors come into play that make it easier for one person to become obese and another to stay trim his or her whole life.
From diet pills, to body wraps to hypnosis, we have invented, created and crafted a multitude of measures to shed unwanted pounds. And after psychological and behavioral interventions have been enacted to help someone lose weight, in steps the medical community to take a scientific stab to drop those extra pounds that too many of us carry around.
According to the National Institute of Diabetes and Digestive and Kidney Diseases, in cases of severe obesity, treatment through diet and exercise alone fall short of assisting in significant weight loss. One of the ways that medicine has tried to help obese individuals is through surgery.
Gastric bypass surgery is one such popular procedure made famous by Al Roker, Star Jones and about 150,000 additional individuals each year. Recently, other forms of weight loss surgeries, often referred to as bariatric surgery, have also been created. Despite the differences between the styles of procedures, according to the Mayo Clinic, in general, all bariatric procedures alter the anatomy of the digestive system thereby controlling or limited the amount of food that can be eaten and digested.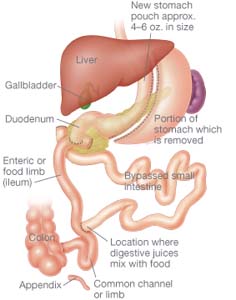
Even though gastric bypass surgery is the most popular form of weight loss surgery, a new procedure called the Duodenal Switch, or Biliopancreatic Diversion, has been an increasingly popular choice among patients and doctors.
Just like other bariatric procedures, the surgery is not just for anyone who needs to lose a few pounds. In order to qualify for the having the operation performed, you must be at least 100 pounds over their normal weight and have a Body Mass Index (BMI) of 40 or more. If you have a BMI between 35 and 40, you must also have weight-related health problems such as diabetes, high blood pressure, heart disease, breathing problems, sleep apnea, high cholesterol or a few other degenerative conditions.
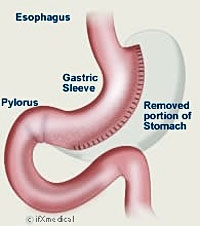
Duodenal Switch surgery is an effective weight-loss surgery that differs from gastric bypass in several ways. Rather than bypassing part of the stomach, about 75 percent of the stomach is removed. This drastic reduction in stomach size greatly limits the amount of food a person can eat in one setting. The small intestine is also shrunk so that the amount of fat and calories that are absorbed from food is greatly reduced.
Like any bariatric surgery, the surgery itself is just one element. It is by no means a cake-walk to a svelte self. Following surgery, blood clotting, hair loss, and loose stools are all common side effects. Individuals with Duodenal Switch surgery must follow a high-protein diet and lifelong vitamin and mineral supplementation to prevent nutrient deficiency.
For many who have had success with this surgery, they have learned to appropriately manage these potential consequences. And the benefits of losing weight, even if it means a drastic change in how and what a person eats, make it worth it.
Even though insurance companies are beginning to cover more and more weight-loss surgeries, many insurance companies still consider the Duodenal Switch procedure to be experimental and may therefore offer no monetary assistance toward it. If you are curious about it, talk to your primary care physician first and then inquire with your health insurance company.